In the 1990s under the leadership of Dr. David W. Chambers, the school led the nation in the adoption of a competency-based education model for pre-doctoral dental programs. In contrast to the prevailing system of ‘clinical requirements,’ an approach that merely counted a pre-set number of procedures completed in each clinical discipline, competency implies an ongoing and broad-based measure of the developing knowledge, skills, abilities, and values essential to the beginning practice of general dentistry. In a competency-based model, multiple faculty observers repeatedly evaluate independent student performance in a natural setting over time.
These competency statements were developed in 2016-17 by a representative group of faculty, students, and alumni to reflect the ‘head, heart and hands’ philosophy the school embraces:
- the integration of current and emerging biomedical and clinical knowledge (head);
- professionalism, ethical behavior, empathy, and communication skills (heart);
- and clinical skills (hands).
Goal of the Educational Program

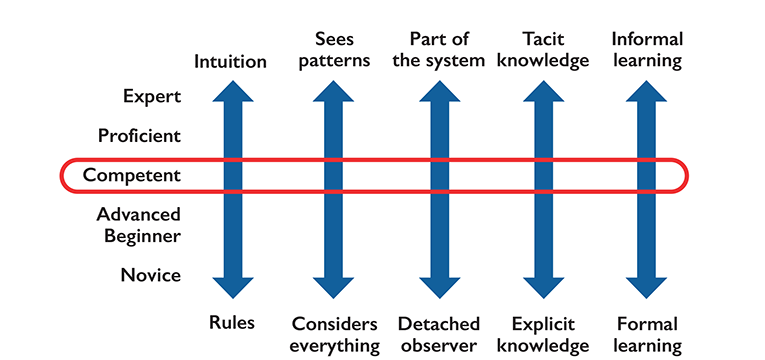
Patricia Benner, Novice to Expert Continuum
Competency Statements
Competence (competency): knowledge, skills, abilities, and values essential to the beginning practice of oral health care that are performed consistently and independently in natural settings. Competence is observable over time and therefore can be measured and assessed to ensure acquisition.
Competencies
- Integrate biomedical science and clinical knowledge to improve oral and systemic health.
- Think critically; use the scientific method to evaluate established and emerging biomedical and clinical science evidence to guide practice decisions.
- Recognize manifestations of systemic disease and evaluate the impact on oral health, oral health care, and well-being.
- Recognize and evaluate the impact of comprehensive oral health care on systemic health and well-being.
- Apply the principles of health promotion and disease prevention to individuals and communities.
- Apply the principles of bioethics to practice.
- Apply the principles of behavioral science to practice.
- Establish and maintain trust and rapport with all stakeholders in patient care. Demonstrate empathy.
- Manage the oral health care needs of pediatric, adolescent and adult patients, including geriatric patients and patients with complex needs.
- Perform comprehensive diagnostic evaluations and risk assessment on patients at all stages of life.
- Obtain, select, and interpret images and tests necessary for accurate differential diagnoses and correlate them with clinical findings.
- Formulate and present comprehensive, sequenced treatment plans and prognoses in accordance with patient needs, values and expectations.
- Obtain and document informed consent or refusal.
- Follow standard infection control guidelines.
- Preserve and restore hard and soft tissue to support health, function and aesthetics:
- Screening and risk assessment for head and neck cancer;
- Local anesthesia and pain and anxiety control;
- Appropriate utilization of therapeutic and pharmacological agents used in patient care;
- Management of orofacial pain;
- Communicate with dental laboratory technicians and manage laboratory procedures to support patient care;
- Risk assessment, prevention and management of caries, including minimally invasive dentistry;
- Restore and replace teeth, including operative, fixed, removable and dental implant therapy;
- Risk assessment, prevention, and management of periodontal disease, including recare strategies;
- Dental emergencies;
- Pulpal therapy and endodontics;
- oral mucosal, temporomandibular and osseous disorders;
- Bony and soft tissue surgery;
- Malocclusion and space management; and
- Evaluate treatment outcomes, prognosis, and continuing care strategies.
- Recognize and manage medical emergencies in the dental setting.
- Interact effectively with stakeholders from diverse cultures, backgrounds and identities.
- Practice, delegate, or refer within the scope of practice and in alignment with patient needs, values, and expectations.
- Apply current principles of business, financial and human resource management to lead the oral health care team.
- Evaluate contemporary and emerging models of oral healthcare delivery, understand dentistry's role in the larger health care system and strive to reduce barriers to care.
- Collaborate with the interprofessional health care team to improve oral-systemic health, enhance the patient experience and reduce risk.
- Evaluate and implement current and emerging technology to diagnose, prevent and treat disease.
- Engage in ongoing quality assurance to improve patient outcomes.
- Behave professionally: manage personal behavior and performance in accordance with standards of the school and the profession.
- Practice in accordance with current local, state and federal laws and regulations.
- Demonstrate ongoing reflection, self assessment, continuous learning and professional development.
- Demonstrate healthy coping and self care strategies.
- Participate in professional activities to promote the profession and serve individuals and communities.
(final, approved by curriculum committee, Jan. 25, 2018)
Definitions
Biomedical science: the scientific knowledge base of human biology required for the treatment and prevention of oral and systemic disease. This includes knowledge of anatomy, biochemistry, molecular and cell biology, epidemiology, embryology, genetics, histology, immunology, microbiology, nutrition, pathology, pharmacology, physiology, and related knowledge domains.
Critical thinking: the ability to interpret, evaluate, and draw sound conclusions in sometimes complex situations where all information may not be present or apparent. In professional practice, critical thinking is the application of rational analysis to patient assessment, diagnosis, and treatment planning. The practitioner must be able to identify pertinent information, make decisions based on deliberate review of options, evaluate outcomes of diagnostic and therapeutic tests or decisions, and assess his or her own competence and ability.
Evidence-based dentistry (EBD): an approach to oral health care that requires the judicious integration of clinically relevant scientific evidence relating to the patient's oral and medical condition and history, the dentist's clinical expertise, and the patient's treatment needs and preferences. (American Dental Association).
Oral health: a functional, structural, aesthetic, physiologic, and psychosocial state of well-being that is essential to an individual’s general health and quality of life (ADA House of Delegates, 2014).
Prevention: procedures, processes, or strategies that reduce risk, promote disease prevention, and result in improved patient health.
Bioethics: the shared discipline of reflective examination of ethical issues and implications in health care, health science, and health policy.
Behavioral science: a branch of science that studies human action and investigates decision-making processes and communication strategies that occur within and between organisms in a social system. Familiarity with major concepts of the discipline may provide solutions to an array of individual, family, and community challenges.
Stakeholder: any person or party in the healthcare setting with an interest in the financing, implementation, or outcome of a service, practice, process, or decision made by another. Stakeholders include patients, care givers, family members, faculty and other practitioners, specialists, the dental school, and others consulting on or providing care.
Empathy: to understand the thinking, perspectives, and feelings of others. To be done correctly, empathy requires interest in others and a set of skills.
Complex needs: patients with moderate to severe medical, developmental, and/or psychosocial conditions that require of the practitioner additional information or knowledge to manage the patient’s health.
Stages of life: pediatric (< 14 years), adult (15-65 years), older adults (66-84), and oldest old (>85), including the frail elderly and patients with complex needs.
Identity: the belief that a subject, person, or thing is the same as it is represented or claimed to be. Identity can encompass race, gender, sexual orientation, gender identity, age, ability, and other personal characteristics.
Scope of practice: procedures, treatments, and actions that a practitioner is allowed to undertake as prescribed by professional licensure and that are within the practitioner’s competence.
Oral health care team: generally composed of the dentist, specialist dentist, dental therapist or dental health aide therapist, dental hygienist (with or without expanded function), dental assistant (with or without expanded function), office support staff, and the dental laboratory technician. Physicians, nurses, nurse practitioners, physician assistants, and other medical professionals are increasingly a critical component of the team.
Interprofessional education: When students from two or more health professions learn about, from, and with each other to enable effective patient care collaboration and improve health outcomes. Interprofessional collaborative practice exists when providers from different health backgrounds work together with patients, families, caregivers, and communities to deliver quality care (adapted from the World Health Organization, 2010).
Patient experience: all elements of the care experience that contribute to patient satisfaction: scheduling, reception, treatment and care, sensitive and empathetic interactions with staff and providers, billing, and follow up.
Quality assurance: systematic and ongoing assessment and evaluation of the quality and appropriateness of a service, product, process, structure, or outcome. The process involves identifying strengths and weaknesses, designing and implementing solutions or strategies to improve performance, and careful monitoring to determine the effectiveness of a change or intervention.
Professionalism (see also 2017 ADEA Statement on Professionalism in Dental Education): the habitual and judicious use of communication skills, knowledge, technical skills, clinical reasoning, empathy, values, and reflection in daily practice for the benefit of the individual or community being served. (Epstein RM, Hundert EM. Defining and assessing professional competence. JAMA 2002: 287: 226–235). Professionalism is the foundation of the doctor-patient relationship. It requires integrity and a high level of skill. The professional assumes an obligation to sharpen and develop skills and judgment throughout a career.
Reflection: the active process of reviewing, analyzing, and evaluating experiences, drawing upon theoretical concepts or previous learning, to inform future action (Reid, 1993).
Self-Assessment: the evaluation of one’s performance against current, defined, evidence-based standards and, ultimately, without external input.
Self-Care: activities and practices that are engaged in regularly that aim to reduce stress and to maintain and enhance health and well-being. Prioritizing emotional, physical, intellectual, occupational and environmental wellness is necessary to honor professional and personal commitments. Healthy self-care includes a realization of when to reach out for help or support.
General dentistry: (a) the evaluation, diagnosis, prevention, and surgical and non-surgical treatment of diseases, disorders and conditions of the oral cavity, maxillofacial area, and the adjacent and associated structures, and their impact on the human body; (b) a service provided by a dentist within the scope of his/her education, training, and experience; and that is (c) in accordance with the ethics of the profession and applicable law. A general dentist is an integral part of the healthcare system and is the primary oral health care provider for patients of all ages. (adapted from ADA House of Delegates, 1997).
Scientific method: the foundation of the natural sciences that comprises some or all of the following: (a) systematic observation, measurement, and experimentation; (b) induction and the formulation of hypotheses; (c) the making of deductions from the hypotheses; (d) the experimental testing of the deductions; and (e) the modification of the hypotheses, if necessary.
Terms updated March 10, 2021